What are chromogenic bacteria?
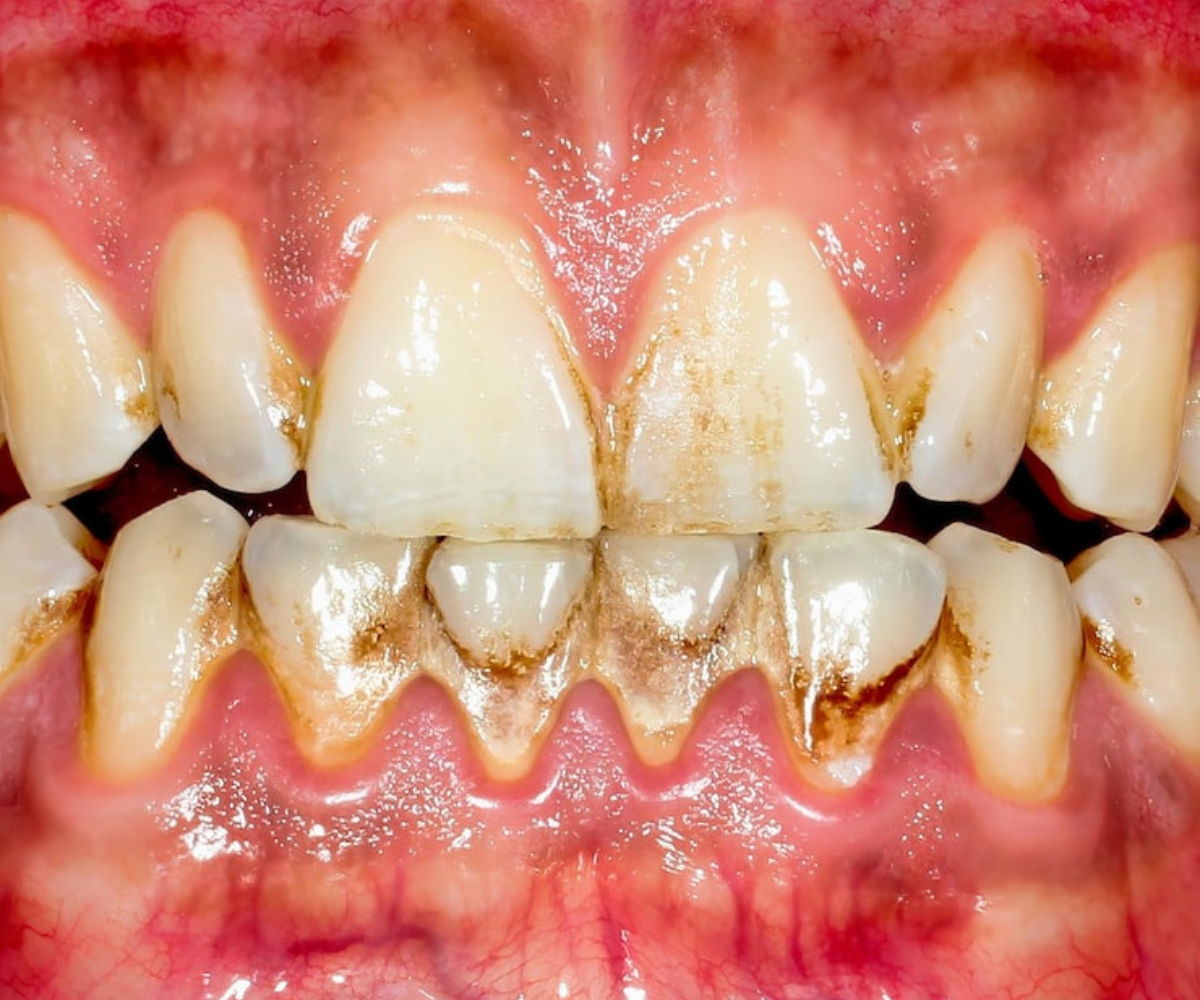
Chromogenic bacteria are oral microbes that produce pigmented metabolites—most often black,
brown, or green pigments—when they metabolize dietary iron, sulfides, or other substrates. The
pigments can bind to the enamel surface, dental plaque, and even the gingival tissues, creating a
characteristic discoloration that is sometimes called “black stain” or “chromogenic staining.”
Common culprits include Actinomyces spp., Prevotella melaninogenica, Porphyromonas gingivalis,
and certain Streptococcus strains.
Causes, Risk Factors & Their Impact on Oral Health
1.How they affect teeth and the oral cavity
- Visible staining – The pigments adhere to the pellicle and plaque, producing a dark, often uneven coloration on the labial surfaces of anterior teeth and, less frequently, on posterior teeth.
- Plaque retention – Pigmented biofilm can be more tenacious, encouraging further plaque accumulation and increasing the risk of gingivitis or early periodontal breakdown.
- Aesthetic concerns – Patients frequently seek treatment for the cosmetic impact, especially when the staining is extensive or involves the smile zone.
- Potential link to disease – While the staining itself is not pathogenic, the bacteria that produce the pigments are often associated with periodontal disease and cariespromoting biofilms.
2. Primary causes and risk factors
- Poor oral hygiene – Inadequate plaque control allows chromogenic organisms to proliferate.
- High dietary iron or sulphide intake – Ironrich foods, supplements, or sulphurcontaining beverages (e.g., certain teas, coffee) provide substrates for pigment formation.
Chromogenic Bacteria: Impact on Teeth & How to Control Them
- Smoking and tobacco use – Nicotine and tar promote bacterial colonization and pigment deposition.
- Salivary composition – Reduced flow or altered pH can favour growth of pigmentproducing species.
- Existing periodontal disease – Deep pockets and inflamed tissues create anaerobic niches where chromogenic bacteria thrive.
| Modality | How it Works | Typical Protocol |
|---|---|---|
| Professional prophylaxis | Mechanical removal of plaque and pigment using ultrasonic scaling, hand instrumentation, and polishing. | Full-mouth scaling & root planing followed by high-speed polishing with a prophylaxis paste (e.g., sodium bicarbonate). |
| Topical agents | Chlorhexidine (0.12% or 0.2%) mouth rinse reduces bacterial load; povidone-iodine may be used adjunctively. | Rinse twice daily for 2 weeks, then maintain weekly if needed. |
| Dietary modification | Reducing iron-rich foods/supplements and sulphur-containing drinks lowers bacterial substrate availability. | Counsel patient on diet; advise water-based beverages and balanced nutrition. |
| Improved oral hygiene | Regular brushing and interdental cleaning disrupt biofilm formation and limit recolonization. | Brush twice daily with fluoride toothpaste + floss/interdental brushes; reinforce technique at each visit. |
| Laser or photodynamic therapy (optional) | Targets pigmented bacteria directly, reducing recolonization. | Single session of diode laser (810 nm) or antimicrobial photodynamic therapy; evidence still emerging. |
| Antibiotic therapy (rare) | Systemic antibiotics only when refractory cases show signs of active infection. | Short course of amoxicillin-clavulanate or metronidazole; avoid routine use due to resistance. |
Chromogenic Bacteria in the Mouth: Problems & Fixes
The scoping review of 21 studies reported a prevalence of chromogenic staining ranging from 3.1 % to 18.5 %, highlighting that while not ubiquitous, the condition is clinically relevant and often under-reported. The same review emphasized the scarcity of high-quality evidence for management, underscoring the need for individualized, hygiene-focused treatment plans.
Prognosis and long-term plan
- Short-term outcome: With thorough de-staining and reinforcement of oral hygiene, most patients achieve a noticeable improvement within 1–2 weeks.
- Recurrence risk: High if underlying risk factors (poor hygiene, diet, smoking) persist; recurrence rates reported up to 30 % within 6 months in non-compliant patients.
- Maintenance strategy:
- Recall visits every 3–4 months for prophylaxis and reinforcement of hygiene.
- Home care: daily brushing, flossing, and a chlorhexidine rinse for the first month post-treatment.
- Lifestyle counseling: smoking cessation, dietary adjustments, and management of xerostomia if present.
Overall prognosis: Excellent when patients adopt consistent oral hygiene and modify risk factors; poor if habits remain unchanged.